|
|
||||
|
LEAD Action News
Vol 2 no 3
Winter 1994.
ISSN 1324-6011 |
||||
|
About Us
|
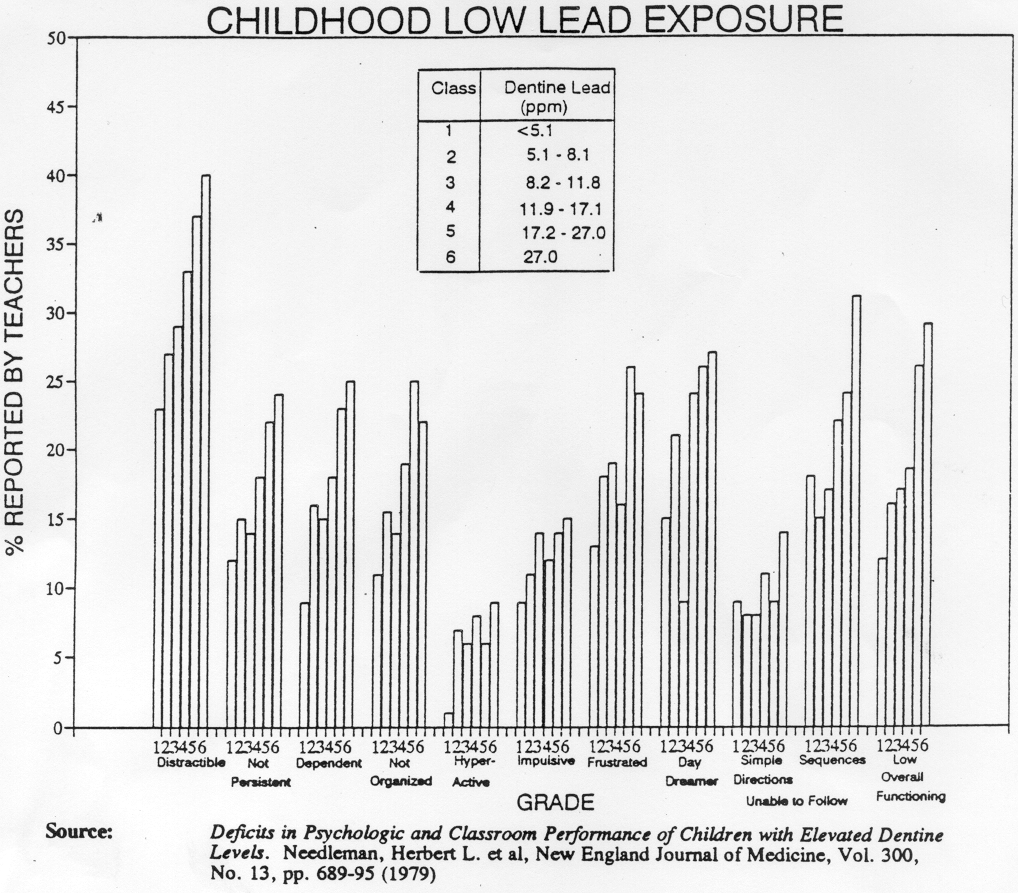
The Early Lead Poisoned Child in the Classroom: Symptomatology and Intervention for School Psychologists and School-Based Personnel By Anne M.W. Winner,
NCSP, C.A.S.E. Symptomatology Lead exposure, in early developmental years, even below treatment levels, may produce deficits in: 1. IQ
2. ATTENTION
3. BEHAVIOUR
4. LANGUAGE/AUDITORY
5. PERCEPTUAL INTEGRATION
INTERVENTION 1. Inquire about lead exposure at school entrance or special education screenings.
2. In the classroom: In regular or special education classes, the child who shows difficulty should have:
FURTHER RECOMMENDATIONS
A WORD FROM THE EDITOR If you’re concerned about a school child after reading the article above, then a simple lead test on the child’s shed baby tooth may set your mind at rest or identify a problem and save recriminations. For some schoolchildren there would be merit in having a blood lead test, but only if the child has some unusual habits eg renovating, making fishing sinkers, sucking toy soldiers, thumb-sucking, nail-biting or pica (eating non-food items). For a child who was only poisoned as an infant, the blood test result will be normal to low, so only the tooth lead result remains as evidence of the lead poisoning. Example of a Report (May 1994): Description: Deciduous Crown – Upper left central incisor. Sample mass = 0.1915 g. Result: 22.2 µg/g (ppm) Comment: In a study published by H T Delves, Southampton General Hospital, UK (1982) the range of lead in deciduous crowns collected from a control group of children was 1.0 to 26.9 µg/g, with a mean of 4.7 µg/g. In personal research (1990) involving a study of 221 deciduous crowns collected from children in the Sydney area the range of lead was: 1.7 to 38.2 µg/g, with a mean of 5.4 µg/g. The frequency distribution of results across this range is skewed, and from the data obtained I would suggest that "normal" values for lead in deciduous crowns range from: 1 to 13.5 µg/g. |
|||
|
About
Us |
bell
system lead poisoning |
Contact Us
| Council
LEAD Project | egroups | Library
- Fact Sheets | Home
Page | Media Releases Newsletters | Q & A | Referral lists | Reports | Site Map | Slide Shows - Films | Subscription | Useful Links | Search this Site |
||||
|
Last
Updated 13 November 2012
|
||||